An extremely rare disease called monkeypox, a cousin of smallpox, has again made its way around the world.
More than 100 cases of monkeypox have been reported in 11 countries across Europe and North America, and in Australia, a rare occurrence for a virus largely confined to central and western Africa.
As of Friday, France, Germany, Sweden and the Netherlands have each confirmed one recent case, Canada has reported two and Belgium and Italy three. The U.K.’s case total is up to 20, Portugal’s 23 and Spain’s 30. Australia reported one case Friday, in a traveler who recently returned from Britain. Most of those countries have more suspected cases awaiting confirmation.
What is monkeypox and where does its name come from?
Monkeypox belongs to the family of poxviruses, which includes smallpox. The disease got its name after scientists found it among laboratory monkeys in 1958. The first monkeypox case in a human was diagnosed in 1970.
Since then, most infections have been concentrated in the Democratic Republic of the Congo and Nigeria. The DRC reports thousands of cases annually and Nigeria has reported more than 200 confirmed cases and more than 500 suspected ones since 2017.
Around 1 percent of people who contract the West African clade die, compared to up to 10 percent of people who contract the Congo Basin clade, according to the World Health Organization.
Monkeypox can spread to people when they come into physical contact with an infected animal. Animal hosts include rodents and primates. The risk of catching monkeypox from animals can be reduced by avoiding unprotected contact with wild animals, especially those that are sick or dead (including their meat and blood). In endemic countries where animals carry monkeypox, any foods containing animal meat or parts should be cooked thoroughly before eating.
According to the WHO,People with monkeypox are infectious while they have symptoms (normally for between two and four weeks). You can catch monkeypox through close physical contact with someone who has symptoms. The rash, bodily fluids (such as fluid, pus or blood from skin lesions) and scabs are particularly infectious. Clothing, bedding, towels or objects like eating utensils/dishes that have been contaminated with the virus from contact with an infected person can also infect others.
Ulcers, lesions or sores in the mouth can also be infectious, meaning the virus can spread through saliva. People who closely interact with someone who is infectious, including health workers, household members and sexual partners are therefore at greater risk for infection.
The virus can also spread from someone who is pregnant to the foetus from the placenta, or from an infected parent to child during or after birth through skin-to-skin contact.
It is not clear whether people who do not have symptoms can spread the disease.
What are the symptoms of monkeypox?
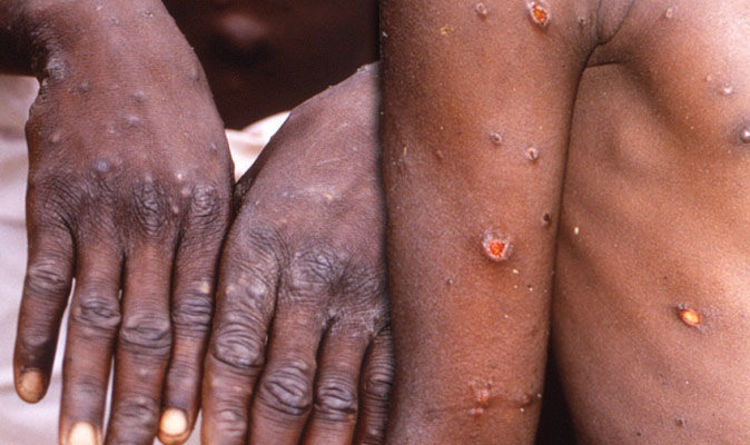
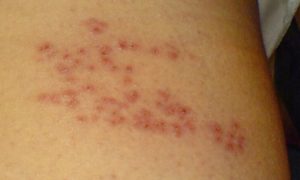
Monkeypox typically starts with flu-like symptoms such as fever, headache, muscle aches and exhaustion. Patients may develop a rash on their face or other parts of the body within one to three days of the fever.
The rash can look similar to chickenpox, syphilis or herpes, but a distinguishing feature is fluid-filled blisters called vesicles on the palms of the hands.
Symptoms can develop anywhere from five to 21 days after someone is infected. Most people recover after two to four weeks.
There are several vaccines available for prevention of smallpox that also provide some protection against monkeypox. A newer vaccine that was developed for smallpox (MVA-BN – also known as Imvamune, Imvanex or Jynneos) was approved in 2019 for use in preventing monkeypox and is not yet widely available. WHO is working with the manufacturer to improve access. People who have been vaccinated against smallpox in the past will also have some protection against monkeypox. The original smallpox vaccines are no longer available to the general public, and people below the age of 40 – 50 years are unlikely to have been vaccinated, since vaccination against smallpox ended in 1980 after it became the first disease to be eradicated. Some laboratory personnel or health workers may have been vaccinated with a more recent smallpox vaccine.
Monkeypox symptoms often resolve on their own without the need for treatment. It is important to take care of the rash by letting it dry if possible or covering with a moist dressing to protect the area if needed. Avoid touching any sores in the mouth or eyes. Mouth rinses and eye drops can be used as long as cortisone-containing products are avoided. Vaccinia immune globulin (VIG) may be recommended for severe cases. An antiviral that was developed to treat smallpox (tecovirimat, commercialized as TPOXX) was also approved for the treatment of monkeypox in January 2022.
You can reduce your risk by limiting contact with people who have suspected or confirmed monkeypox.
If you do need to have physical contact with someone who has monkeypox because you are a health worker or live together, encourage the infected person to self-isolate and cover any skin lesion if they can (e.g., by wearing clothing over the rash). When you are physically close to them, they should wear a medical mask, especially if they are coughing or have lesions in their mouth. You should wear one also. Avoid skin-to-skin contact whenever possible and use disposable gloves if you have any direct contact with lesions. Wear a mask when handling any clothes or bedding if the person cannot do it themselves.
Regularly clean your hands with soap and water or an alcohol-based hand rub, especially after contact with the person who is infected, their clothes, bed sheets, towels and other items or surfaces they have touched or that might have come into contact with their rash or respiratory secretions (e.g., utensils, dishes). Wash the person’s clothes, towels and bedsheets and eating utensils with warm water and detergent. Clean and disinfect any contaminated surfaces and dispose of contaminated waste (e.g., dressings) appropriately.
What's happening in Tunisia?
Subscribe to our Youtube channel for updates.